Cancer Care
Prostate Cancer

The risk of developing prostate cancer increases as a man ages. We offer a wide range of the latest treatment options available.
Prostate cancer is the most common cancer in men in the U.S. other than skin cancer. The risk of developing prostate cancer greatly increases with age. Black American men are at greater risk than white American men, but the reason for this is not known. The cause of prostate cancer is likely complex and based on multiple factors.
As with any cancer, early detection is the key to successful treatment. At Urology of Indiana, we encourage men age 40 and over to schedule a prostate exam and PSA blood test.
Our teams are on the front lines of prostate cancer evaluation and treatment. Urology of Indiana physicians follow the American Urological Association and National Comprehensive Cancer Center’s evidence-based practice guidelines to ensure the highest quality of care.
Within our practice, we provide prostate cancer patients up-to-date access to the latest non-surgical and surgical treatment options, including five highly experienced da Vinci robotic Prostatectomy surgical teams and two radiation therapy centers – known as the Urology of Indiana Integrated Cancer Care Centers (North and South locations).
These specialty centers feature external beam image-guided radiation therapy. Having these centers on-site at Urology of Indiana provides patients with the convenience of having their physician visits and treatments at one location. The integration of our Radiation Oncology Team with our Urologists allows for customized treatment planning and strong continuity of care.
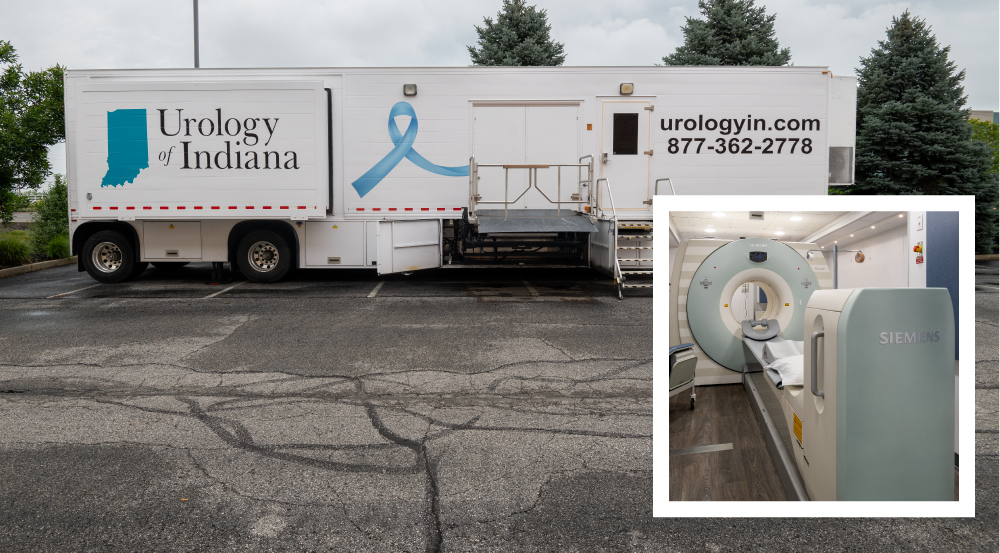
Urology of Indiana Now Offers a Mobile PET-CT Scanner to Help Detect Prostate Cancer!
Early Detection
A family history of prostate cancer in a brother or father significantly increases chances of getting prostate cancer. There is emerging evidence to date that diet, nutrition and obesity may also play a role in developing prostate cancer.
In the early stages of prostate cancer there usually are no symptoms. When symptoms do develop, they vary according to the size and location of the tumor, and are often the same as those for benign prostate conditions. In fact, it is more likely that any of these symptoms would indicate prostate enlargement (known as benign prostatic hypertrophy), infection or other conditions rather than cancer. Still, a physician should check any symptom. Only a physician conducting the proper tests can determine for sure whether the condition is cancerous or benign.
The guidelines related to initiation of screening unfortunately remain variable and somewhat controversial. UOI physicians believe early detection of and risk assessment for prostate cancer should be offered to asymptomatic men 40 years of age or older and those who have a life expectancy of at least 10 years. Men who wish to be screened should have both a prostate-specific antigen (PSA) test and a digital rectal exam (DRE). MRI of the prostate has an increasingly common and important role in the risk assessment for clinically significant prostate cancer. The decision to proceed to prostate biopsy should be based not only on PSA and DRE results but consider multiple factors including free and total PSA, patient age, PSA velocity, PSA density (PSA/Prostate Volume), family history, ethnicity, prior biopsy history and comorbidities.
Diagnosis
When a change is detected in the prostate either by digital rectal exam (DRE) or rising PSA, a prostate MRI and/or biopsy may be recommended to determine the presence of cancer. MRI-CAD (computer assisted diagnostics) is now emerging as a very helpful diagnostic tool. MRI imaging allows radiologists and urologists to “peer inside” the prostate and get additional information about the size and any suspicious areas within the prostate and pelvis. When suspicious areas exist within the prostate, Artemis MRI/Ultrasound Fusion biopsies can be performed to target the suspicious areas.
This exciting technology allows the Urologist to overlay (or Fuse) the real-time ultrasound images with the MRI-CAD. Any suspicious areas can then be targeted with great accuracy. This technique has been shown to increase detection rates of clinically significant prostate cancer and is an important tool. In addition, MRI/Ultrasound Fusion biopsy of the prostate has an emerging role in monitoring and managing patients who have already been diagnosed with prostate cancer and are on Active Surveillance.
A prostate biopsy involves removal of small tissue samples that are examined under a microscope and is the ONLY way to determine conclusively the presence of prostate cancer. The tissue samples are obtained by inserting an ultrasound probe into the rectum to visualize the prostate on a monitor. If a fusion biopsy is performed, the MRI images are integrated into the ultrasound platform to guide biopsy location. A thin needle is then placed through the probe into the prostate. This procedure is known as needle biopsy. The brief procedure can be performed in the office or surgery center with either local and/or light sedation.
At Urology of Indiana, we offer a wide range of the latest options available for the treatment of prostate cancer including active surveillance, robotic prostatectomy and radiation therapy. We have dedicated teams of physicians and health providers that specialize exclusively in the management of prostate cancer. Our focus and specialization allow for the best possible outcomes.
Active Surveillance
Active Surveillance (AS) is offered for appropriate men who have been diagnosed with Low-Risk prostate cancer. AS involves serial monitoring of the PSA and digital rectal exam. MRI imaging, genetic testing and repeat biopsy are employed to reduce the chance of initial under staging of the cancer at diagnosis and to monitor for any progression of the cancer to intermediate or higher risk disease. With progression of cancer, men are then eligible for definitive treatment with surgery or radiation therapy.
Radical Prostatectomy
Radical prostatectomy is the surgical removal of the prostate gland and surrounding tissues, including the seminal vesicles +/- the pelvic lymph nodes. Traditionally, surgeons used one of two surgical techniques, including retropubic prostatectomy or perineal prostatectomy. More commonly, radical prostatectomy is now performed robotically.
Robot-Assisted Laparoscopic Prostatectomy
The modern surgical approach is robot-assisted laparoscopic surgery — better known as da Vinci prostatectomy. This minimally invasive technique increases the surgeon’s precision by enhancing the ability to perform complex minimally-invasive surgery. Benefits include shorter hospital stay, less post-operative pain, less blood loss, faster recovery and quicker return to work.
Image Guided Radiation Therapy (IGRT)
Radiation therapy uses high-energy particles or waves, such as x-rays, gamma rays, electrons or protons to destroy or damage cancer cells. It is one of the most common treatments for cancer.
Special equipment delivers high doses of radiation to cancerous cells, killing or damaging them so that they cannot grow or spread. Although some normal cells may be affected by radiation, most recover fully from the effects of the treatment. Unlike chemotherapy, which exposes the entire body to cancer-fighting chemicals, radiation therapy is a local treatment and affects only the part of the body being treated.
Radiation therapy treatment is a coordinated team effort. Our radiation therapy team of medical professionals at our Integrated Cancer Care Centers will care for you throughout your course of treatment.
SpaceOAR Hydrogel For Patients Undergoing Radiation
Urology of Indiana offers SpaceOAR Hydrogel. This is the first and only FDA-cleared spacer to help reduce the radiation dose delivered to the rectum of men undergoing radiation treatment for prostate cancer. SpaceOAR is designed and applied to reduce rectal complications and help patients to maintain their quality of life after radiation treatment.
SpaceOAR is an absorbable gel inserted via a minimally invasive injection and creates a temporary space between the prostate and the rectum. It is performed in the office setting at Urology of Indiana, allowing us to complement the patient’s radiation treatment to better target their cancer while preserving healthy tissue. The hydrogel spacer remains in place for about three months. After about six months, the hydrogel is naturally absorbed and cleared from the body in the patient’s urine.
SpaceOAR is an important advance that reduces radiation dose to the rectum during radiation treatments to help prevent unwanted side effects. We understand that men diagnosed with prostate cancer may have some difficult decisions to make regarding their treatment, but knowing that an option like SpaceOAR Hydrogel can help limit the risk of damage to other organs during radiation treatment will hopefully make a few of those decisions easier.
UroPlan: A Roadmap For Return to Sexual Function After Cancer
There is much more to a man’s life than his cancer diagnosis. As a result, we believe preserving and maintaining quality of life to be an essential component of comprehensive cancer care. By helping patients prepare for surgery with a solid strategy for recovery, we know that we’re able to offer men their best chance to experience a satisfying outcome.
UroPlan by Urology of Indiana uses a “stepwise” approach to facilitate recovery of both sexual and urinary function following cancer treatment. The recovery rate after surgery is highly individualized.
Many factors such as desire for sexual activity, partner interest, pre-treatment sexual function, existing medical conditions and the presence of anxiety or depression can greatly influence the recovery process. Therefore, the roadmaps we follow should be considered a starting point.
Our Care Team will optimize and customize the program for each man, as the pace of recovery and return to sexual activity varies significantly for each patient. Our Timeline and Roadmap Choices will help guide your recovery.
There are three elements of the UroPlan Consultation:
- Decision is made to proceed with surgery
- Assessment is made of current sexual function, activity level and interest in restoration
- Patient and Surgeon decide upon choice of Restoration Roadmap Program
Roadmap 1: Active Restoration
Roadmap 2: Passive Restoration
Roadmap 3: No Restoration
View Our UroPlan Brochure
For more detailed information about UroPlan, read our brochure here.
View Our UroPlan Video
View our UroPlan video with Urology of Indiana Men’s Health Physician, Alex Tatem, MD.
